Diabetes mellitus (DM) is a metabolic disorder that is characterized by high blood sugar levels caused by an absolute or relative lack of insulin. Diabetes‘ chronic hyperglycemia is linked to long-term injury, dysfunction, and failure of various organs, especially the eyes, kidneys, nerves, heart, and blood vessels.
Insulin is the hormone that regulates intermediate metabolism. The most noticeable immediate consequence is a reduction in blood glucose levels. Diabetes mellitus is caused by decreased (or absent) insulin secretion, which is also accompanied by decreased sensitivity to its action, a condition known as “insulin resistance,” which is closely linked to obesity.
Page Contents
TYPES OF DIABETES
There are three types of diabetes mellitus: type 1, type 2, and gestational diabetes.
- Type 1 diabetes (also known as insulin-dependent diabetes mellitus (IDDM) or juvenile-onset diabetes).
- Type 2 diabetes (also known as maturity-onset diabetes or non-insulin-dependent diabetes mellitus—NIDDM)
- Prediabetes is a disorder in which blood sugar levels are elevated but not high enough to be diagnosed as type 2 diabetes. While not everybody with prediabetes develops type 2 diabetes, a significant number of people do.
- Gestational Diabetes Mellitus (GDM) is a form of diabetes that causes high blood glucose levels during pregnancy and is linked to complications for both the mother and the infant. GDM normally goes away after birth, but it increases the risk of type 2 diabetes in women and their children later in life.
CAUSES
TYPE 1 DIABETES MELLITUS
Type 1 diabetes has an uncertain etiology. The pancreas’ insulin-producing (islet, or islets of Langerhans) cells are usually mistakenly destroyed by the body’s own immune system, which is designed to combat dangerous bacteria and viruses.
Other factors to consider are:
- Genetics
- Viruses and other variables in the ecosystem
- Toxic chemicals
- Cytotoxins
TYPE 2 DIABETES MELLITUS
- Insulin resistance develops in muscle, fat, and liver cells. These cells don’t take in enough sugar because they don’t deal with insulin normally.
- The pancreas cannot produce enough insulin to keep blood sugar levels in check.
- PCOS (Polycystic ovarian syndrome).
PREDIABETES
Precisely what causes prediabetes is unclear. However, it appears that family history and genetics play a significant role. A lack of daily physical activity, as well as being overweight with excess fat around the belly, seem to be significant contributors.
GESTATIONAL DIABETES
The placenta releases hormones to keep the pregnancy going during pregnancy. Insulin resistance is increased in your cells as a result of these hormones.
Your pancreas normally reacts by producing enough extra insulin to overcome this resistance. However, the pancreas can’t always keep up. When this occurs, too little glucose enters your cells and too much remains in your blood, causing Gestational Diabetes.
SYMPTOMS
Diabetes symptoms include
- increased thirst and urination,
- weakness,
- blurred vision,
- numbness or tingling in the feet or hands.
- Unhealed sores
- unexplained weight loss
- feeling more hungry
Other signs and symptoms
- Dry and itchy skin, yeast infections, or urinary tract infections regularly in females.
- Reduced sex drive, erectile dysfunction, and muscle strength in males.
Type 1 diabetes symptoms can appear suddenly, in as little as a few weeks. Type 2 diabetes symptoms frequently appear gradually over many years and are so minor that you might not even recognize them. Type 2 diabetes affects a large number of people who have no symptoms. Some people don’t realize they have diabetes until they start experiencing symptoms like blurred vision or heart attacks.
While pre-diabetes shows no symptoms and in the case of gestational diabetes symptoms are usually undetectable. Between 24 and 28 weeks of pregnancy, the obstetrician will screen you for gestational diabetes.
DIAGNOSIS
Diabetes is diagnosed using the tests mentioned below:
FASTING BLOOD GLUCOSE
A fasting plasma glucose test assesses your blood glucose levels after you have gone without food for at least 8 hours. This test is used to determine whether or not you have diabetes or prediabetes.
It is common to have a fasting blood sugar level of less than 100 mg/dL (5.6 mmol/L). Prediabetes is described as a fasting blood sugar level of 100 to 125 mg/dL (5.6 to 6.9 mmol/L). You have diabetes if the blood sugar levels are 126 mg/dL (7 mmol/L) or higher on two different tests.
ORAL GLUCOSE TOLERANCE TEST
An oral glucose tolerance test (OGTT) tests your blood sugar after you’ve fasted for at least eight hours and drank a glucose-containing beverage for two hours. This test can be used to determine whether or not you have diabetes or prediabetes.
In the OGTT, a typical sugar level is less than 140mg/dl; if the sugar level is between 140mg/dl and 199mg/dl, the patient has pre-diabetes; and if the sugar level is 200mg/dl or higher, the patient has diabetes.
RANDOM BLOOD GLUCOSE TEST
Your doctor tests your blood sugar without regard to when you last ate a meal in a random plasma glucose test. This examination is used to diagnose diabetes, but not prediabetes, along with a review of symptoms.
When blood sugar levels are greater than or equal to 200 mg/dl, diabetes is diagnosed.
HbA1c TEST
Fasting is not needed for a hemoglobin A1c (HbA1c) test, which can be used to diagnose or confirm prediabetes or diabetes.
In an A1c test, a typical sugar level is less than 5.7 percent; if the sugar level is between 5.7 percent and 6.4 percent, the patient has pre-diabetes; and if the sugar level is 6.3 percent or higher, the patient has diabetes.
TREATMENT
Diabetes treatment aims to keep blood glucose levels as close to normal as possible while remaining healthy. People with diabetes must be own responsibility for their treatment daily. This includes blood glucose tracking, food management, physical activity maintenance, weight and stress management, oral drug monitoring, and, if necessary, insulin injections or pump use.
FOOD MANAGEMENT
There is no such thing as a diabetes diet, contrary to common belief. However, it’s important to focus your diet on:
- Meal and snack schedules that are consistent
- Smaller portion sizes
- Fruits, nonstarchy vegetables, and whole grains are rich in fiber.
- There are fewer processed grains, starchy vegetables, and sweets on the menu.
- Low-fat dairy, low-fat meats, and fish in small portions
- Olive oil or canola oil are good cooking oils.
- Lower calorie intake
PHYSICAL ACTIVITY
Exercising is crucial for weight loss or keeping a healthy weight. It also aids in the control of blood sugar levels. The American Diabetes Association (ADA) recommends 30 minutes of moderate-to-vigorous exercise five days a week.
Exercise can aid in the reversal of diabetes in its early stages and the prevention of heart-related complications in more advanced cases.
Aerobic exercise will help you lose weight, lower your blood sugar, and increase your insulin sensitivity. The following examples are given below;
- Brisk walk
- Cycling
- Climbing stairs
- Dancing
- Any sports
- Gardening
- Swimming
Strength training is also beneficial since it improves the amount of glucose the body burns when it is at rest. There are the following activities that increase the muscle strength
- Lifting weights, whether with tools, free weights, or household items, will help you gain muscle strength.
- Bands of resistance
- Squats, push-ups, and lunges are examples of calisthenics.
- High-intensity tasks, for example, gardening
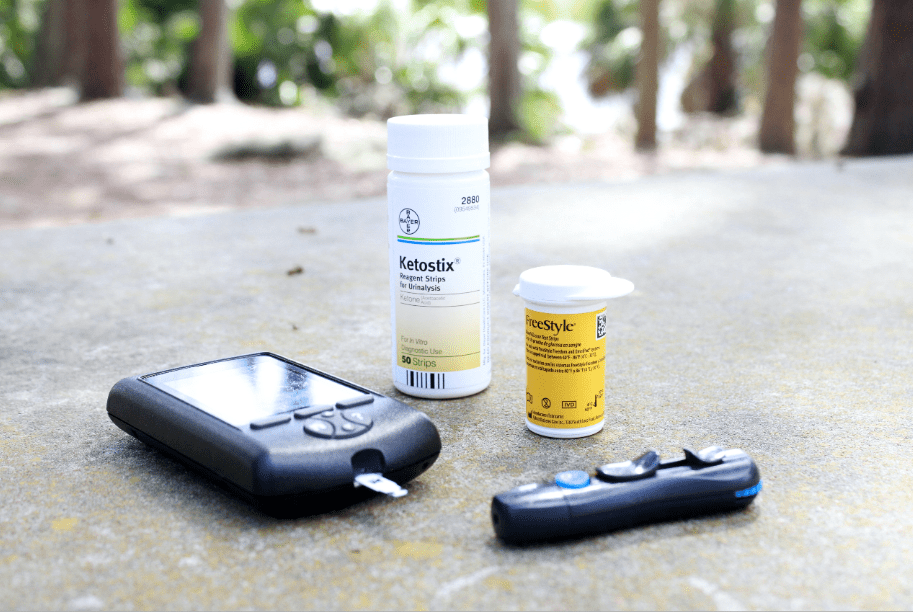
If ketones are found in the urine, it means the body is consuming fat rather than glucose. Since the body cannot tolerate high amounts of this waste product, excess ketones can be extremely harmful.
If ketones are detected in the urine, do not exercise.
WEIGHT LOSS
Weight loss leads to improved blood sugar, cholesterol, triglyceride, and blood pressure regulation. If you’re overweight, you might notice a difference in these variables as soon as you lose 5% of your body weight. The greater the benefit to your health and disease control, though, the more weight you lose.
BLOOD GLUCOSE TRACKING
A blood glucose meter, a small at-home device that monitors the amount of sugar in a drop of your blood, is typically used for monitoring. Keep track of your measurements so you can share them with your doctor.
DIABETES MEDICATIONS
If diet and exercise alone aren’t enough to keep your blood sugar levels in check, your doctor can prescribe diabetes medications that lower insulin levels or insulin therapy. The following drugs are used to treat diabetes.
TYPE 1 DIABETES MELLITUS
Since your body no longer produces insulin, you must take insulin if you have type 1 diabetes. Insulin must be taken many times during the day, including with meals. An insulin pump, which delivers small, consistent doses during the day, is another choice.
TYPE 2 DIABETES MELLITUS
Some people with type 2 diabetes can control their condition by eating healthier foods and getting more exercise. Many people with type 2 diabetes often need diabetes medications.
A chosen medication can have several advantages (for example, lower blood sugar and control cholesterol). Diabetes can be managed with a variety of drug combinations. Not every drug for type 2 diabetes will help every patient, and not every drug is appropriate for every patient.
The drugs for type 2 diabetes are classified into different groups depending on how they function to regulate blood sugar levels.
ORAL ANTIHYPERGLYCEMIC DRUGS:
BIGUANIDES
Metformin & Extended-release metformin are now available that
- decrease hepatic glucose output
- lower fasting glycemia
- reduce HbA1c by 1.5%
ADVERSE EFFECTS:
lactic acidosis, gastrointestinal disturbances
SULFONYLUREAS
- 1st generation no longer used: Chlorpropamide Tolbutamide
- 2nd generation: Glyburide, Glipizide, Glimepiride
- enhance insulin secretion
- lower HbA1c by 1.5 %
ADVERSE EFFECTS:
- hypoglycemia
- weight gain
MEGLITINIDE ANALOGS
- Repaglinide
- Nateglinide
- enhance insulin secretion (early-phase insulin release)
- lower HbA1c by 0.1- 2.1 % (repaglinide) and by 0.2- 0.6% (nateglinide)
SIDE EFFECTS:
- weight gain,
- hypoglycemia
THIAZOLIDINEDIONES (TZDS)
- Rosiglitazone & Pioglitazone
- peroxisome proliferator-activated receptor γ modulators (PPAR γ)
- insulin sensitizers (increase the sensitivity of muscle, fat, and liver to endogenous and exogenous insulin)
- lower HbA1c by 0.5 – 1.4 %
ADVERSE EFFECTS:
- weight gain,
- fluid retention
DPP-IV INHIBITORS
- Sitagliptin: DPP-IV inhibitor
- Dipeptidyl peptidase IV (DPPIV) is a ubiquitous enzyme that deactivates a variety of bioactive peptides, including GIP and GLP-1
- Used alone or in combination with metformin or TZDs
- Reduces HbA1c by 0.5 – 0.7 %
ADVERSE EFFECTS:
- increased rate of respiratory infections,
- headaches
a-GLUCOSIDASE INHIBITORS
- Acarbose
- Miglitol
- reduce the rate of digestion of polysaccharides in the proximal small intestine, primarily lowering post-prandial glucose level
- slower HbA1c by 0.5 – 0.8 %
ADVERSE EFFECTS:
- increased gas production
- gastro-intestinal symptoms
INSULIN THERAPY
- Rapid-acting insulin starts working 15 minutes after injection, peaks in an hour and works for another 2 to 4 hours.
- Regular or short-acting insulin usually enters the bloodstream within 30 minutes of injection, peaks between 2 and 3 hours after injection, and lasts for 3 to 6 hours.
- Intermediate-acting insulin enters the bloodstream 2–4 hours after injection, peaks 4–12 hours later, and lasts 12–18 hours.
- Long-acting insulin takes several hours to enter the bloodstream and appears to reduce glucose levels evenly over 24 hours.
if you have any comments/suggestions about this article ” Everything You Need to Know About Diabetes” or want to know more about Diabetic complications then do write to us.